Gerbode defect
Gerbode defect
Gerbode defect
Gerbode defect is
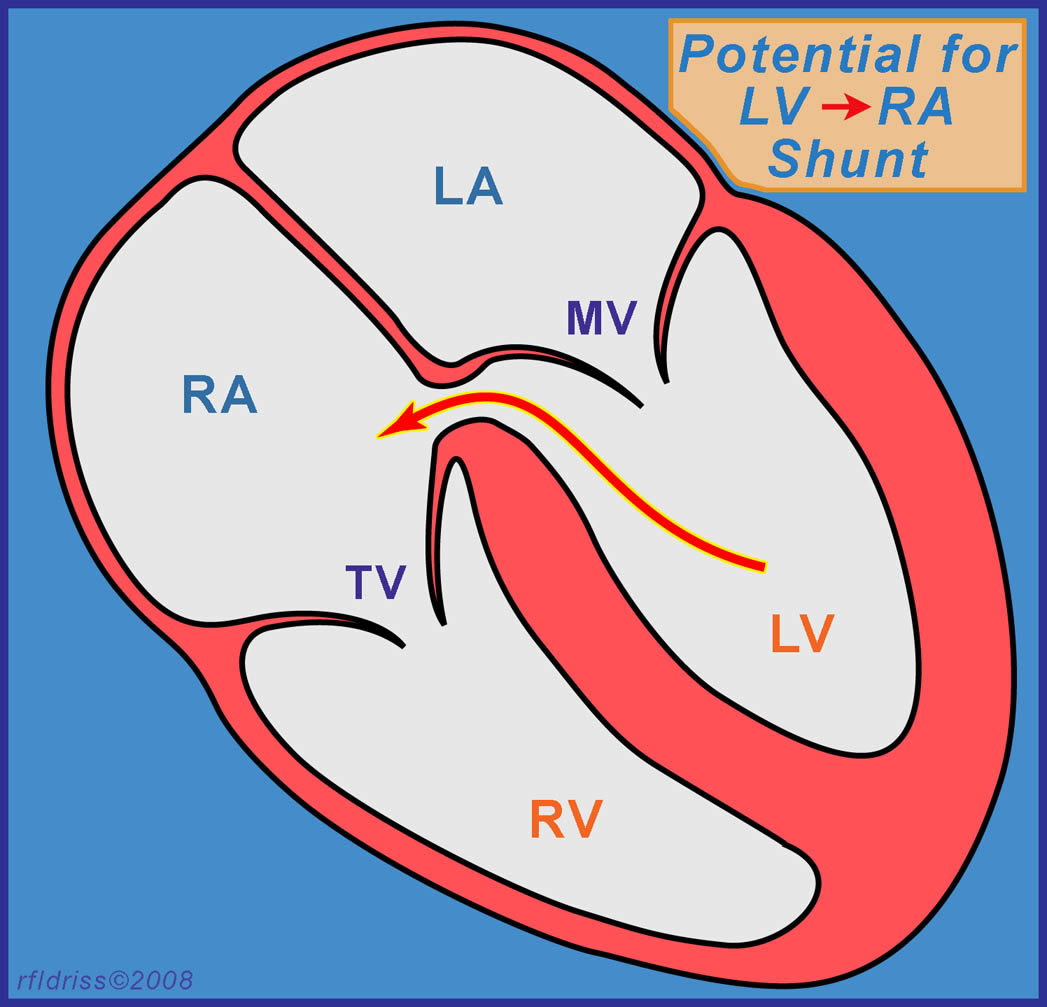
[A] Shunt between LV and LA
[B] Shunt between LV and RA
[C] Shunt between LA and RA
[D] Shunt between LV and RV
Gerbode defect
Gerbode Defect – Overview
🔹 Definition
A Gerbode defect is a rare type of ventricular septal defect (VSD) where there is an abnormal communication between the left ventricle (LV) and the right atrium (RA).
- First described by Gerbode in 1958.
- Accounts for <1% of all congenital cardiac defects.
🔹 Types
- Congenital – due to embryological maldevelopment of membranous septum.
- Acquired – following:
- Infective endocarditis
- Valve surgery (esp. tricuspid or aortic valve replacement)
- Trauma
- Myocardial infarction
🔹 Anatomy
- The membranous septum has two parts:
- Interventricular portion (between LV & RV)
- Atrioventricular portion (between LV & RA)
A defect in the atrioventricular portion allows direct LV → RA shunt.
🔹 Hemodynamics
- Normally: LV pressure >> RA pressure
- In Gerbode defect → blood flows from LV (high pressure) into RA (low pressure)
- Produces left-to-right shunt → RA and RV volume overload
🔹 Clinical Features
- Symptoms depend on shunt size:
- Small defect → asymptomatic
- Large defect → dyspnea, fatigue, right heart failure signs
- Murmur:
- Classically a loud pansystolic murmur best at the lower left sternal border
- Can mimic tricuspid regurgitation murmur
🔹 Diagnosis
- Echocardiography (TTE/TEE with Doppler)
- Shows high-velocity systolic jet from LV → RA
- Differentiates from tricuspid regurgitation (jet direction is opposite)
- Cardiac catheterization
- Step-up in O₂ saturation at the RA level
- MRI/CT (rarely needed)
🔹 Complications
- Right-sided heart failure
- Pulmonary hypertension (long-standing cases)
- Endocarditis
- Arrhythmias
🔹 Management
- Small/asymptomatic → sometimes observation
- Moderate–large defects or symptomatic patients →
- Surgical closure (preferred for congenital or large acquired defects)
- Percutaneous device closure (select cases, especially acquired small defects)
🔹 Prognosis
- Excellent with timely repair
- Delay → right heart dilation, pulmonary hypertension, heart failure
✅ In summary:
A Gerbode defect is an LV–RA shunt, often congenital but can be acquired after endocarditis or surgery. It presents with a loud pansystolic murmur, diagnosed best by Doppler echo, and usually requires surgical or device closure if significant.
Gerbode defect
- Gerbode defect
- Abnormal shunting between the left ventricle and right atrium
- congenital defect or prior cardiac insults.
- Most prevalent cause of Gerbode defect – congenital
- Acquired cases has recently been reported
Gerbode defect – Characteristic murmur
- LV-RA shunt is a similar to that of a VSD: loud, harsh pansystolic
- Grade III–VI
- Unvarying with respiration
- Often associated with a thrill along the left sternal border
Gerbode defect murmur – Differentiate from VSD
- VSD murmurs can have a higher frequency quality
- Varies with respiration
- Becoming softer during inspiration
Diagnostic procedure of choice
- Transesophageal echocardiography (TEE)
Echocardiographic findings suggesting Gerbode defect
- (1) atypical jet direction
- (2) persistent shunt flow into diastole
- (3) lack of ventricular septal flattening
- (4) no right ventricular hypertrophy
- (5) normal diastolic pulmonary artery pressure as estimated from the pulmonic regurgitant velocity.
Explanation
Gerbode defect shows a high-velocity jet from LV to RA, unlike tricuspid regurgitation where flow originates in RA and jets into RV.Explanation
The atrioventricular portion of the membranous septum separates LV from RA. Defect here produces direct LV–RA communication.Explanation
Both Gerbode defect and tricuspid regurgitation produce pansystolic murmurs along left sternal border.Explanation
LV–RA shunt increases O₂ saturation in RA, not RV.Explanation
Infective endocarditis can erode the membranous septum, producing an acquired Gerbode defect.Explanation
Gerbode defect causes right-sided volume overload and pulmonary hypertension, not systemic embolism.Explanation
Blood flows from LV (high pressure) to RA (low pressure), creating a left-to-right shunt.Explanation
TEE provides detailed visualization of membranous septum defects and high-velocity jets.Explanation
Large symptomatic Gerbode defects require surgical closure to prevent right heart failure and pulmonary hypertension.Explanation
With timely repair, Gerbode defect carries excellent prognosis and patients usually lead normal lives.1. What is the simplest definition of a Gerbode defect?
LV → RA communication (left ventricle to right atrium shunt) across the atrioventricular membranous septum.
2. Which murmur does a Gerbode defect commonly produce?
A harsh pansystolic murmur at the lower left sternal border that can mimic tricuspid regurgitation.
3. What echocardiographic sign strongly suggests Gerbode defect?
A high-velocity systolic color Doppler jet originating from the LV side of the membranous septum and entering the RA.
4. Which invasive test confirms the diagnosis by oxygen saturations?
Cardiac catheterization showing an early oxygen saturation step-up at the right atrial level.
5. Name two common acquired causes of Gerbode defect.
Infective endocarditis and iatrogenic injury during aortic/tricuspid valve surgery (also trauma or myocardial rupture).
6. When should closure be considered?
For symptomatic patients, Qp:Qs ≥1.5, progressive RA/RV dilation, hemolysis, or endocarditis—anatomic suitability considered for device vs surgical repair.
7. Which modality best delineates anatomy before intervention?
Transesophageal echocardiography (TEE) with 3D imaging for precise defect location and rim assessment.
8. What common diagnostic pitfall should clinicians avoid?
Mistaking the LV→RA jet for severe tricuspid regurgitation—always trace the jet origin and direction on multiple echo views.
9. What are the main hemodynamic consequences of an untreated significant Gerbode defect?
Right atrial and right ventricular volume overload, progressive right-sided dilation, and eventual pulmonary hypertension if long-standing.
10. What is the usual prognosis after successful repair?
Excellent — most patients have near-normal life expectancy and symptomatic improvement when treated timely.
| # | Key Point |
|---|---|
| 1 | Gerbode defect = LV→RA communication; <1% of congenital defects. |
| 2 | Classified as direct (supravalvular) vs indirect (infravalvular). |
| 3 | Anatomic site: AV portion of membranous septum (direct type). |
| 4 | Acquired causes: valve surgery injury, infective endocarditis, trauma. |
| 5 | Hemodynamics: LV systolic pressure » RA → high-velocity systolic jet. |
| 6 | Murmur: harsh pansystolic at LLSB; may not obey Carvallo’s sign. |
| 7 | Echo hallmark: systolic color jet from LV side crossing into RA. |
| 8 | Common pitfall: misdiagnosed as severe TR; track jet origin. |
| 9 | Continuous-wave Doppler often >4 m/s; can overestimate RVSP if mistaken for TR. |
| 10 | Catheterization: earliest O2 step-up at RA. |
| 11 | Chronic significant shunt: RA/RV dilation; eventual PH if untreated. |
| 12 | Indications for closure: symptoms, Qp:Qs ≥1.5, RV/RA dilation, hemolysis, endocarditis. |
| 13 | Surgery preferred for large/complex defects or poor rims. |
| 14 | Device closure feasible in small-moderate, well-rimmed, non-valve-adjacent defects. |
| 15 | TEE/3D echo sharpens anatomy and rim relationships pre-intervention. |
| 16 | Differentiate from TR: jet direction/origin; inspiration response may differ. |
| 17 | Associated lesions: perimembranous VSD, septal aneurysm, tricuspid anomalies. |
| 18 | Post-repair residuals: color Doppler TTE across multiple views is sensitive. |
| 19 | Complications: right heart failure, PH, arrhythmias, endocarditis. |
| 20 | Prognosis excellent with timely repair; delayed treatment worsens outcomes. |